The year in review
In 2019, the Ebola outbreak declared in northeastern Democratic Republic of Congo (DRC) in August 2018 continued to rage, alongside the worst-ever measles epidemic, while further east, two cyclones, and severe flooding devastated parts of Mozambique, Sudan, and South Sudan.
There was an upsurge in conflict across the Sahel and in Yemen, and thousands of migrants, refugees, and asylum seekers remained trapped in Libya, Greece, and Mexico, exposed to violence and disease.
Doctors Without Borders (MSF) teams responded to all these crises, and other emergencies around the world, during the year, with a workforce of approximately 65,000 people – around 80 percent of whom were hired in the countries where we work.

The deteriorating situation for people and relief providers
Living conditions, including access to medical care, significantly deteriorated for many people in countries across the Sahel region – especially Mali, Niger, and Burkina Faso – during 2019. Armed groups and intercommunity violence have made parts of the region extremely insecure and forced people to flee their homes.
MSF provided care to address the immense medical needs, including worrying levels of malnutrition and malaria, particularly among children. However, intense violence and the ever-present threat of abductions meant that it was no longer safe for our teams to work in some areas.
We worked where it was safe to do so, although the precarious context requires a lot of time and staff resources to manage the risks, restricting who and where we are able to help.
In the northwest and southwest Cameroon, where violence between government forces and separatist armed groups escalated sharply, MSF teams extended their activities. The conflict has displaced over 500,000 people since 2016, leaving them in dire need of humanitarian assistance.
In Yemen, where the war entered its fifth year, people are still dying from preventable diseases, due to the collapse of both the economy and the health system. An MSF report released in 2019 showed that a significant number of expectant mothers and sick children had died because of the delay in receiving care.
Though the rate of airstrikes slowed in 2019, the fighting that has torn the country apart continued to rage on many of the frontlines. We struggled to provide relief in a context characterized by insecurity and bureaucratic restrictions imposed in Yemen’s north.
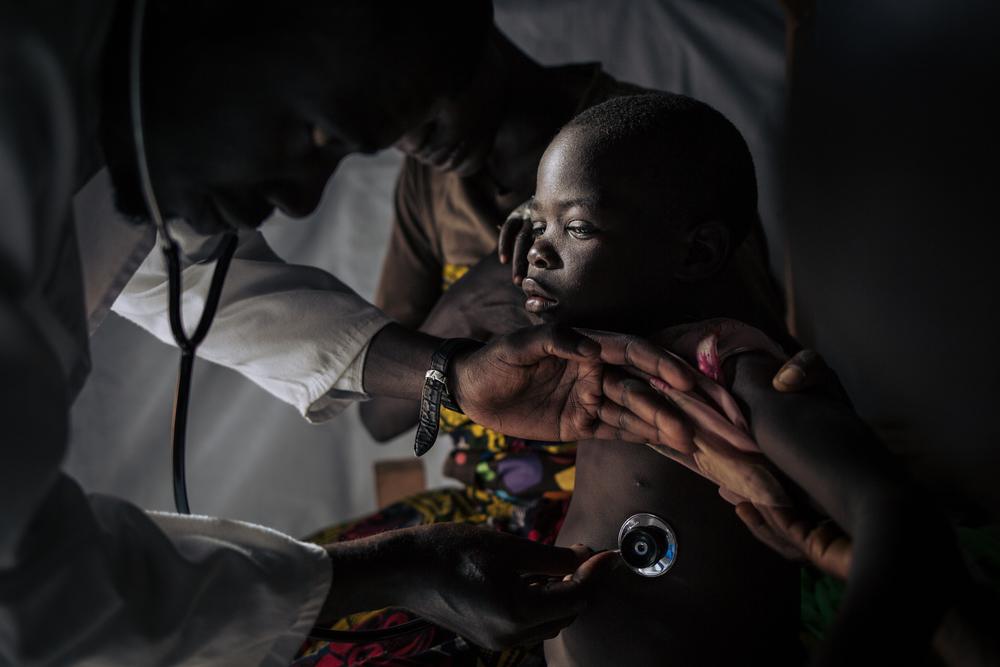
In the Central African Republic (CAR), there were numerous attacks against civilians and civilian infrastructure in 2019. In late May, gunmen shot dead more than 50 people they had brought together under the pretence of organising a community meeting.
The conflict severely limited access to medical care: when MSF teams came to administer vaccines in Mingala town, residents had not seen a doctor or humanitarian worker for more than two years.
Millions of people driven from their homes in war-torn Syria are still living in unsafe and precarious conditions in camps. Our efforts to deliver assistance to them were severely hampered in 2019, not only by insecurity but also by administrative challenges.
MSF is working on obtaining registration to work in Syria and has not been authorized by the government of Syria to have direct access in some areas. Part of our medical aid supplies for northern Syria are normally routed through Turkey, a country in which we haven’t been able to renew our registration, rendering the provision of support for our Syrian operations significantly more challenging.
In October, due to the Turkish military operation in northeast Syria, we were forced to reduce our presence or withdraw teams from several locations, including Tal Kocher, leaving vulnerable people with limited access to healthcare. Ain Issa displaced person camp was entirely dismantled, leaving people to seek safety once again.
MSF teams also reduced our presence in both Raqqa city and in Al-Hol camp, where 70,000 people – 94 percent of whom are women and children – are held.
Against all odds, we still maintain a presence in Syria and try to provide assistance where possible; much of our work is in supporting medical networks and local hospitals, which are able to provide some level of care to people.
However, we are not currently able to work in the country to the level that we would like, and that also meets people’s needs.

Responding to epidemics
Large-scale measles outbreaks swept across several countries during 2019, resulting in thousands of deaths. DRC was particularly hard hit, with 310,000 cases reported and around 6,000 deaths, three-quarters of them children under the age of five.
In one week alone in November, nearly 10,000 cases were recorded across the country.
Yet the epidemic has attracted very little international attention and funding; by August, only R41.53 million out of the required R149.50 million had been raised for the UN-led response plan. In DRC, MSF launched activities in 16 provinces, vaccinating over half a million children and treating more than 30,000 patients.
Our intervention has not been without its challenges, however; insecurity, vaccine stockouts, and logistical issues have hindered operations in some areas.
MSF also responded to measles outbreaks in Cameroon, Nigeria, Chad, and Lebanon, conducting vaccination campaigns and setting up new measles wards in health facilities.
By the end of the year, the Ebola outbreak in northeastern DRC had claimed over 2,200 lives. Despite the lessons learned from the West Africa epidemic and the availability of two new vaccines and investigational treatments, two-thirds of infected people died.
MSF was frustrated with the slow, opaque, and restricted vaccination efforts, leaving MSF vaccination teams on standby for weeks, while we publicly called on the World Health Organization for greater vaccine supply transparency.
Our teams continued to tackle the disease in North Kivu and Ituri provinces but insecurity and the failure to gain people’s trust impeded activities. Two of the Ebola treatment centres we ran in North Kivu were attacked and burned down within days of each other in February.

Responding to natural disasters
In March, a weather system dumped heavy rain on Malawi, leading to severe flooding, before heading out to sea and developing into Cyclone Idai, which hit Mozambique first, and then Zimbabwe. Around 80 percent of Beira town in Mozambique was destroyed in the storm.
MSF launched a large-scale intervention to provide medical care, conduct water, and sanitation activities, rebuild damaged health facilities, and assist local authorities to contain a cholera outbreak, including through vaccination campaigns.
In October, parts of South Sudan, Sudan, and Somalia were severely affected by floods. South Sudan was hard hit, with hundreds of thousands of people displaced and unable to meet their most basic needs. The price of food tripled, making it unaffordable for many.
In the eastern town of Pibor, the MSF hospital flooded and had to move, before the new area also flooded, significantly reducing our lifesaving activities and access to healthcare for people.

Assistance to migrants and asylum seekers
Migrants and asylum seekers continued to be abandoned, neglected, or pushed back by authorities across the world. From Central America to the Horn of Africa, our teams see the suffering of people on the move.
While MSF was able to resume our Mediterranean search and rescue operations in August with a new boat, the Ocean Viking, thousands of migrants were trapped in Libya in a context of increasing violence. When conflict broke out in Tripoli in early April, many remained locked up and abandoned in detention centres.
On 2 July, two airstrikes hit the Tajoura detention centre, killing at least 53 people.
In Europe, governments continue to sit on their hands while migrants trying to flee Libya are picked up and returned there by EU-funded Libyan coastguards, and thousands of people languish in miserable conditions on the Greek islands.
MSF teams treat people in both places, including those with severe mental health issues that have developed as a result of their plight.

Medical advocacy in action
2019 marked 20 years since MSF was both awarded the Nobel Peace Prize and established the Access Campaign with the subsequent prize money.
During the last two decades, the Access Campaign’s advocacy work for more affordable and accessible drugs has enabled MSF to scale up treatment for a number of diseases, including HIV, hepatitis C, and tuberculosis.
Twenty years after the then-MSF president Dr. James Orbinski delivered the Nobel Prize lecture, the words in his speech still resonate:
“As an independent volunteer association, we are committed to bringing direct medical aid to people in need. But we act not in a vacuum, and we speak not into the wind, but with a clear intent to assist, to provoke change, or to reveal injustice.”
We are grateful to our donors whose support makes our work possible, and to all MSF staff working in our programmes, who give their time and skills to assist others at often considerable risk to themselves. Our thoughts remain with Romy, Richard, and Philippe, our colleagues abducted in DRC in July 2013, who are still missing.
